Subtotal $0.00
Introduction
Gallstones, medically called cholerhiasis, are a common digestive condition affecting millions of people worldwide in 2026. When the digestive fluid (bile) in the gallbladder gets out of balance, it hardens into small, stone-like deposits. While some people never notice symptoms, others experience sudden and intense pain in the upper right abdomen, especially after eating fatty meals. Because the gallbladder plays an important role in digestion, any blockage in bile flow can lead to discomfort, nausea, and sometimes serious complications.
The good news is that gallstones are highly treatable with modern medical care. Simple tests like ultrasound can quickly detect the problem, and treatment options range from monitoring mild cases to safe, minimally invasive surgery. Understanding the causes, symptoms, risk factors, and prevention strategies is essential for protecting your digestive health. This article explains everything you need to know about cholerhiasis in clear, easy-to-understand language, based on the latest 2026 medical guidance.
What Are Cholerhiasis?
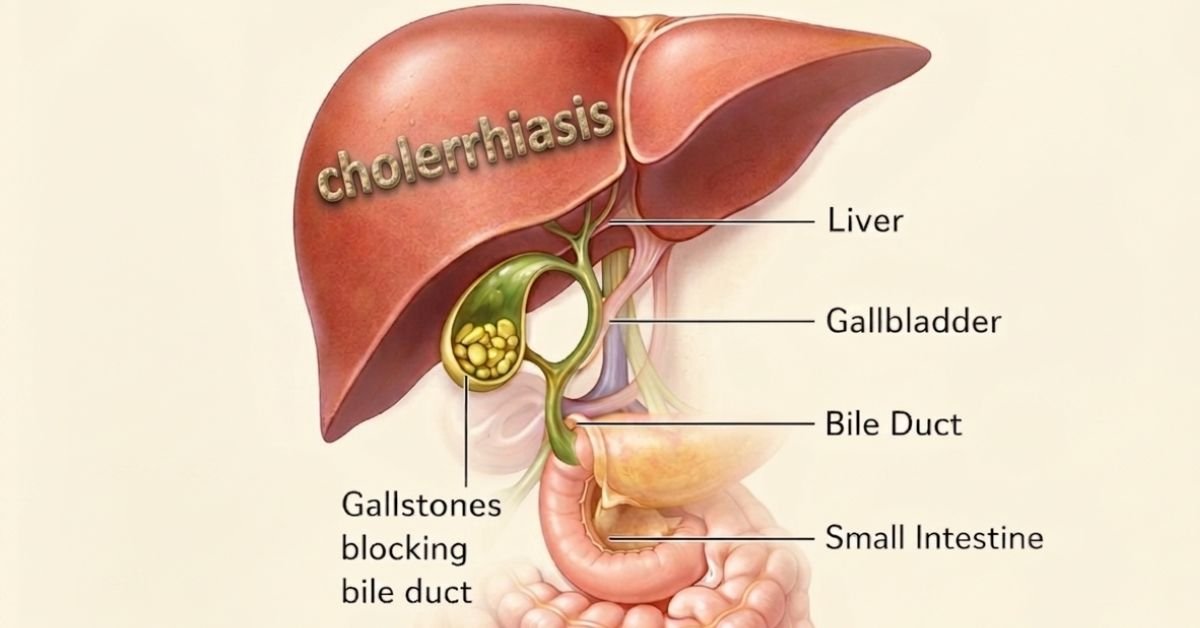
The gallbladder is a small organ located under your liver on the right side of your abdomen. Its job is to store bile, which helps digest fats. Occasionally, the chemicals in bile become unbalanced. When that happens, they can harden into solid pieces. These tough pieces are called gallstones.
They can be:
- As small as a grain of sand
- As large as a golf ball
Some people have just one stone. Others may have many.
Quick Definition
Cholerhiasis is a medical condition where rigid stones form in the gallbladder and may block bile flow, causing pain and digestion problems. Many cases are “silent,” meaning no symptoms appear. But when a stone blocks a bile duct, it can cause sudden and severe pain.
How Do Gallstones Form?
Gallstones usually form slowly over time. They develop when bile contains too much of certain substances.
Main Causes of Stone Formation
- Too much cholesterol in bile
If the liver releases more cholesterol than bile can dissolve, crystals form. These crystals can grow into stones. - Too much bilirubin
When red blood cells degrade, bilirubin is created. For every course, a student may make folders. Certain liver or blood conditions increase bilirubin levels, leading to stone formation. - Gallbladder doesn’t empty properly
When bile stays in the gallbladder too long, it becomes concentrated and thick, increasing the risk of stones.
Think of it like sugar in tea, if you add too much and don’t stir, it settles and forms crystals at the bottom.
Types of Gallstones
Not all gallstones are the same. They differ based on what they are made of.
| Type of Gallstone | Main Component | Common In | Color |
| Cholesterol Stones | Hardened cholesterol | Most adults in Western countries | Yellow-green |
| Pigment Stones | Bilirubin | People with liver or blood disorders | Dark brown/black |
| Mixed Stones | Combination | Many patients worldwide | Mixed colors |
According to 2026 gastroenterology reports, cholesterol stones constitute about 80% of cases. Pigment stones are more common in people with:
- Liver disease
- Sickle cell anemia
- Certain infections
Common Symptoms
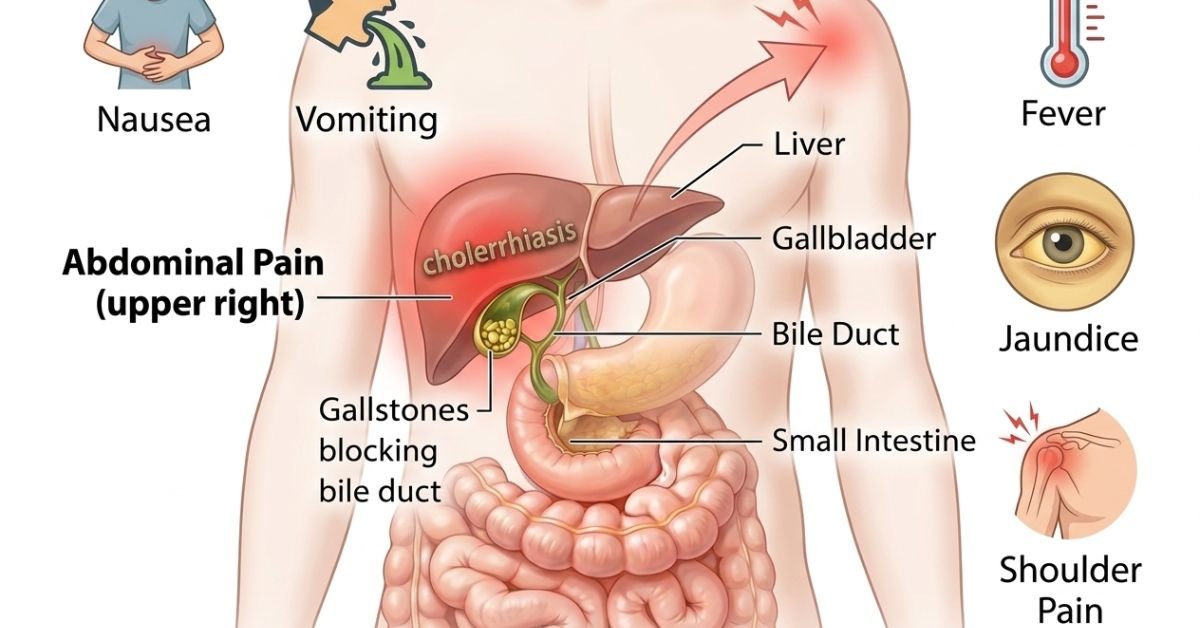
Many people with gallstones have no symptoms at all. But when a stone blocks a bile duct, symptoms can appear suddenly.
Typical Signs
- Sudden pain in the upper right abdomen
- Pain radiating to the right shoulder or back
- Nausea or vomiting
- Feeling bloated after eating fatty foods
- Fever (if infection develops)
- Yellowing of skin or eyes (jaundice)
This painful episode is called biliary colic.
The pain often
- Starts after a heavy or greasy meal
- Lasts 30 minutes to several hours
- Stops suddenly when the stone moves
Emergency Warning
Seek immediate medical help if you have severe pain with fever and yellow skin. This may mean infection or a blocked bile duct.
Who Is at Risk?
Some people are more likely to develop gallstones.
Major Risk Factors
- Being female
- Age over 40
- Overweight or obesity
- Rapid weight loss
- High-fat, low-fiber diet
- Diabetes
- Family history
- Pregnancy
- Hormonal medications (like birth control pills)
Doctors sometimes remember the common risk group with the phrase:
Healthy lifestyle choices can reduce risk, even if you have some of these factors, such as maintaining a balanced diet, exercising regularly, and managing weight effectively.
How Doctors Diagnose Gallstones
If a doctor suspects gallstones, they may order tests to confirm.
Common Tests
- Ultrasound – Most common test; painless and quick
- Blood tests: Look for liver issues or infections
- CT scan – Detailed images of the abdomen
- MRI (MRCP) – Shows bile ducts clearly
- HIDA scan – Checks gallbladder function
Ultrasound is usually enough to detect gallstones.
Doctors choose tests based on:
- Symptoms
- Severity
- Possible complications
Treatment Options
Treatment depends on whether symptoms are present.
No Symptoms (Silent Gallstones)
Doctors usually recommend
- Monitoring
- No immediate treatment
Many people live their entire lives without problems.
Symptomatic Gallstones
If pain or complications occur, treatment is needed.
Surgery (Cholecystectomy)
- Most common treatment
- Gallbladder is removed
- Usually done with small cuts (laparoscopic surgery)
- Recovery time: 1–2 weeks
You can live normally without a gallbladder. The liver still makes bile.
Medication
- Ursodiol can dissolve small cholesterol stones.
- Takes months to work
- Not suitable for all patients
Shock Wave Therapy
- Breaks stones into small pieces
- Rarely used today
Surgery is considered the safest and most effective long-term solution.
Gallstones vs. Gallbladder Inflammation
Gallstones and gallbladder inflammation (cholecystitis) are related but different.
| Feature | Gallstones | Gallbladder Inflammation |
| Cause | Stone formation | Stone blocking gallbladder |
| Pain | Comes and goes | Constant severe pain |
| Fever | Rare | Common |
| Urgency | Sometimes urgent | Often emergency |
| Treatment | Monitor or surgery | Usually urgent surgery |
If gallstones block the gallbladder for too long, infection and swelling can occur. This condition needs immediate medical attention.
Diet and Lifestyle Tips for Prevention
You can lower your risk by making smart daily choices.
Eat More Of
- Fruits and vegetables
- Whole grains
- Beans and lentils
- Healthy fats (olive oil, nuts)
- Lean proteins
Eat Less Of
- Fried foods
- Fast food
- Sugary drinks
- Processed snacks
- Excess red meat
Healthy Habits
- Maintain a healthy weight
- Lose weight slowly (avoid crash diets)
- Exercise at least 30 minutes daily
- Stay hydrated
A 2026 report from the World Gastroenterology Organization shows that people who follow a Mediterranean diet have fewer gallstone complications.
When Should You See a Doctor?
Not every stomachache is serious. But some signs need medical care.
See a doctor if
- Pain keeps returning after meals
- Pain lasts longer than 4 hours.
- You feel frequent nausea.
Go to emergency care if
- Severe abdominal pain
- Fever and chills
- Yellow skin or eyes
- Extreme weakness
Ignoring symptoms can lead to serious problems, like:
- Bile duct infection
- Pancreatitis
- Gallbladder rupture
Early diagnosis prevents complications.
FAQs
Can gallstones disappear naturally?
Rarely. Most require monitoring or treatment.
Is surgery safe?
Yes. Laparoscopic gallbladder removal is very common and safe.
Can teenagers get gallstones?
Yes, but it is less common. Obesity increases risk.
Can I eat normally after gallbladder removal?
Yes. Most people return to normal eating habits.
Are gallstones life-threatening?
Usually not, but complications can be serious if untreated, such as pancreatitis or cholangitis, which may require surgical intervention.
Conclusion
Gallstones, medically known as cholerhiasis, remain one of the most common digestive conditions worldwide in 2026. While many people live with silent stones and never notice symptoms, others experience sudden and severe pain when bile flow becomes blocked. The good news is that modern diagnostic tools like ultrasound make detection quick and accurate, and treatments, especially minimally invasive gallbladder removal, are safer and more effective than ever. Early recognition of symptoms such as upper right abdominal pain, nausea, or jaundice can prevent serious complications like infection or pancreatitis.
The best protection against gallstones starts with simple daily habits: eating a balanced, fiber-rich diet, maintaining a healthy weight, staying active, and avoiding crash diets. If you notice repeated pain after meals, do not ignore it. Talk to a healthcare professional and get a proper evaluation. With early care, proper treatment, and healthy lifestyle choices, most people manage cholerhiasis successfully and continue living normal, active lives.